Heart diseases are still responsible for 40-50% of deaths in the world.
This article has been published to help every individual, young or old, recognize their own risk of heart disease and understand what they need to do to control it.
Heart failure is a term that indicates that the heart is no longer able to pump oxygen to the tissues. This manifests itself as fatigue, shortness of breath, excessive coughing, and difficulty with daily activities.
The heart is a strong ball of muscle and its job is to constantly pump blood. This is called circulation. Circulation delivers oxygen, but also nutrients. It is used in the tissues and returns as carbon dioxide, and this metabolism product is sent to the lungs to be excreted.
The heart has 4 cavities:
The upper spaces are called Atrium. The lower cavities are called Ventricles.
Blood containing oxygen passes from the left atrium to the left ventricle and is pumped from there to the body.
The blood, which has distributed oxygen to the tissues and contains carbon dioxide, is taken into the right atrium, from there it is pumped to the right ventricle, and from there to the lungs.
In order for the heart to work systematically and correctly, all 4 cavities must work in an organized manner.
Heart failure means that the heart cannot manage this system correctly and cannot meet its workforce.
The heart uses several ways to cope with this situation:
Enlargement of the heart: the heart stretches to contract stronger and thus pump more blood. Over time, this causes the heart to enlarge.
Building more muscle mass: Increasing heart and muscle mass occurs through the expansion and growth of contractile cells.
The heart tries to pump faster: the heart tries to pump faster and increase the output of blood containing oxygen.
The blood vessels narrow and increase the pressure, increasing blood flow to the heart to assist in the pumping process.
The kidneys try to increase the osmotic pressure of the blood by excreting less salt. Naturally, this intensity makes the heart’s work more difficult in the future.
However, all these measures are temporary and unless precautions are taken, this will make the burden on the heart even heavier. These symptoms may be:
Breathlessness, which can be felt even during sleep, called dysapnea, the need to keep the head high when lying down and early fatigue while walking (blood tends to return from the pulmonary veins that bring blood from the lungs to the heart, because the heart is insufficient to pump this blood).
Constant need to cough (fluid accumulation in the lungs).
Swelling in the legs, feet and abdomen (since blood flow from the heart decreases, accumulation occurs in the veins and fluid leaks from the veins to the tissues. The kidney becomes insufficient to maintain salt and water balance due to this pressure)
Feeling of fatigue and inadequacy in normal daily activities (causing insufficient metabolic activity, especially in the muscles, as not enough oxygen can be carried to the tissues through the blood).
Loss of appetite and nausea (digestive problems occur because less blood and oxygen reaches the digestive system).
Convulsion and forgetfulness (change in the amount of elements related to brain metabolism in the blood).
Fast heartbeat (the heart tries to pump faster to keep up with its pumping capacity).
At the end of all these symptoms, atrial fibrillation, defined as an irregular heartbeat, may occur. This may cause irregularities (fibrillation) in the electrical vibrations of the heart atrium.
Again, as a result, chest pain called Angina may be felt. This is a feeling of chest tightness. It can also be felt in the arms, neck, jaw, abdomen, back and shoulders. Although there are no such obvious symptoms, shortness of breath can also manifest itself as a digestive system disorder.
However, before angina occurs, precautions must be taken for underlying heart and circulatory problems. The most important of these is Coronary Artery Disease (CAD). This is characterized by contraction of the coronary arteries.
Angina may also be caused by coronary microvascular disease (spasm of the smallest arteries of the heart).
In both cases, blood cannot pass through the vessels easily, it becomes blocked and oxygen flow stops. This condition is called ischemia. Both conditions are causes of angina.
Emergency conditions such as angina, angina pectoris (the feeling of discomfort caused by narrowed arteries) or unstable angina (decrease in oxygen to the coronary arteries, especially due to cholesterol accumulation and increased blockage with clots) may be encountered (the muscle stops contraction due to the blockage of blood and therefore oxygen to the heart muscle). heart attack), coronary microvascular angina (feeling of discomfort in the chest for 15-20 minutes), variable angina (temporary contraction of the coronary arteries, especially at night and in the morning). These are all signs that precautions should be taken. It indicates the need for immediate medical attention.
The doctor first investigates the underlying causes. These can be increased by genetic reasons (presence of people with heart disease in the family), investigation of blockages that cause vascular occlusion, drug treatments, changes in lifestyles, stress, and blood tests.
operations such as overtaking.
Their further procedures, coronary angiography, cardiac catheterization and computed tomography angiography, are clinical interventions that include the problem and its solution.
However, if a person monitors these factors (such as familial history, high blood fat, rhythm disorders, stress) for awareness purposes, he can continue his healthy life by taking precautions and getting checked by a doctor before more serious symptoms occur.

Self-Conducted Health Check for Heart Disease Risks
ECG (Electrocardiogram): It is the measurement of the electrical activity of the heartbeat. With each beat, an electrical impulse (electric wave) passes through the heart. This allows the muscle to contract and pump blood from the heart. A normal heartbeat shows the contraction rhythms of the atria and ventricles.
The right and left atrium, that is, the upper cavities, are called P waves. This is the first wave. This then turns into a straight line as the impulse passes into the lower spaces. After that, the lower right and left spaces form the other wave. This is called the QRS complex. The last wave, the T wave, is the wave in which the heart muscle returns to normal after the end of this wave. With the data diagram obtained after this process, the time for the electrical wave to pass through the heart cavities and whether this activity is fast or slow are observed. Additionally, depending on whether there is an irregular rhythm in this electrical signal, it is tested whether there is a problem in the area that performs the pumping.
Exercise Test (Stress Test): During the test, you walk on a treadmill and the rhythm of electrical currents during heartbeat is measured and recorded. Thus, the pumping rhythm of the heart muscles is tested as the body works more and more intensively. This test should be performed under the supervision of a cardiologist because a possible heart rhythm disorder may pose a risk during follow-up and intervention may be required. This is also useful for the cardiologist to tell the person the limit on how much exercise they can do.
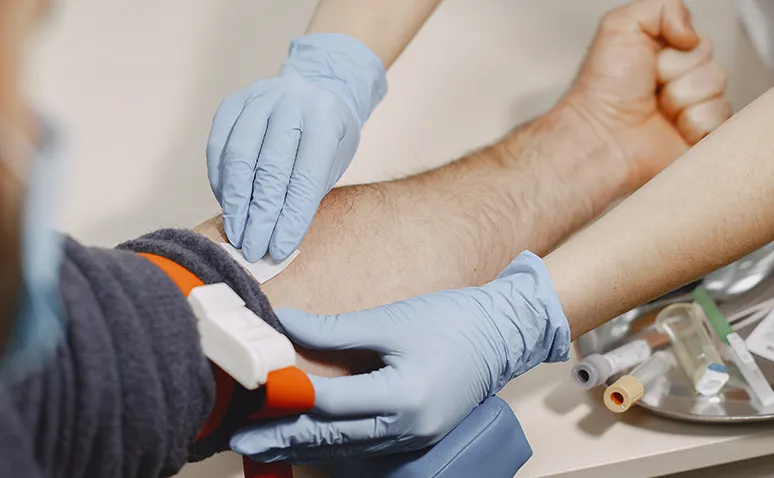
Blood Tests: These tests are performed to understand the precautions that can be taken regarding diet and lifestyle to prevent familial and metabolic risks if there is no heart-related problem, and if there is, to understand the extent of the damage caused by the problem. Blood tests should include:
glucose
HBA1c
troponin
Creatine Kinase
C Reactive Protein (CRP)
fibrinogen
prothrombin
Sedimentation
CBC (whole blood)
homocysteine
triglyceride
Total Cholesterol
HDL Cholesterol
LDL Cholesterol
VLDL Cholesterol
Brain Natriuretic Peptide (BNP)
Sodium
Potassium
Chlorine
Chest X-ray: It is the imaging of the heart, lungs and chest bones with x-rays. It provides information about the location, size and structure of the heart, the condition of the lungs and some blood vessels.
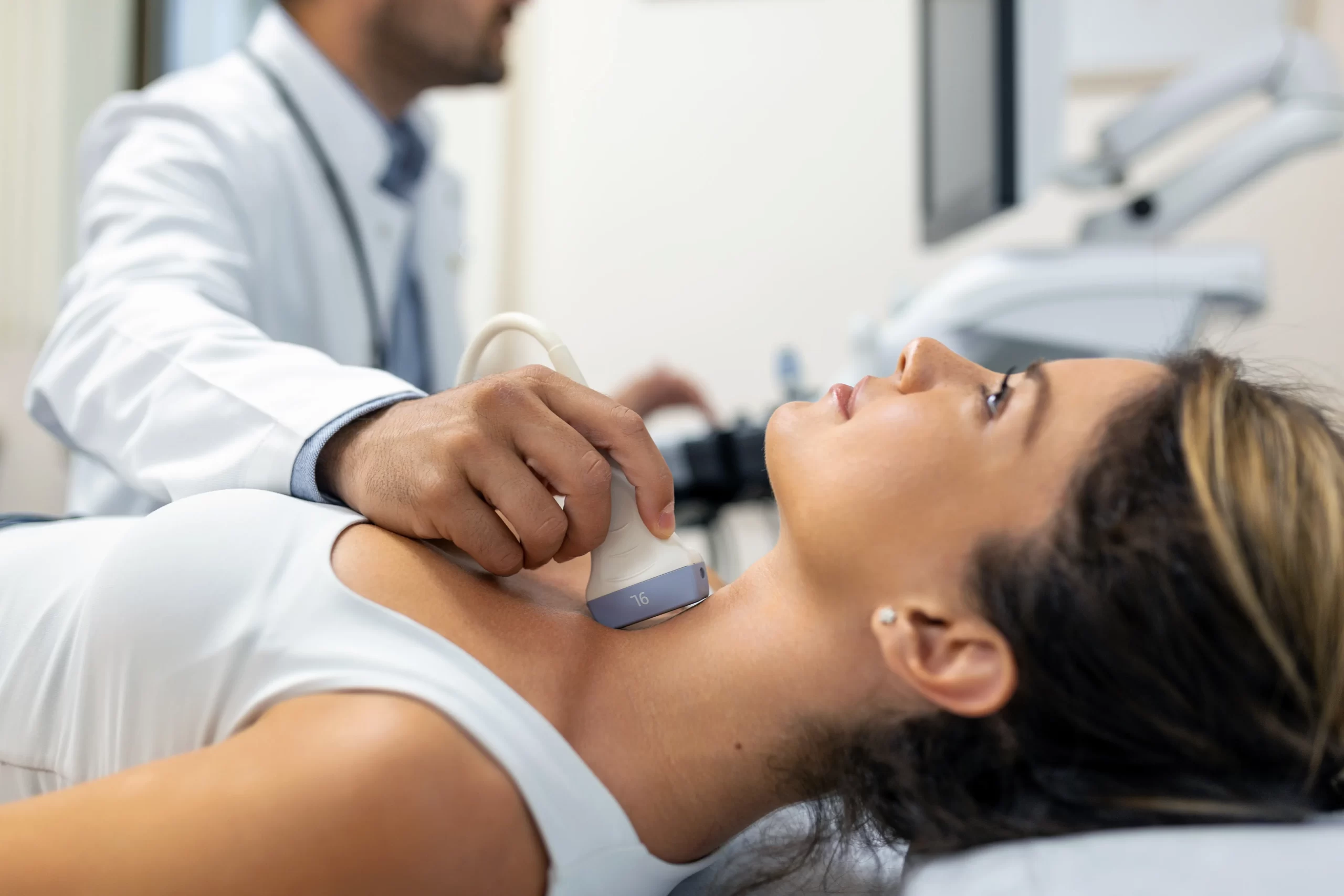
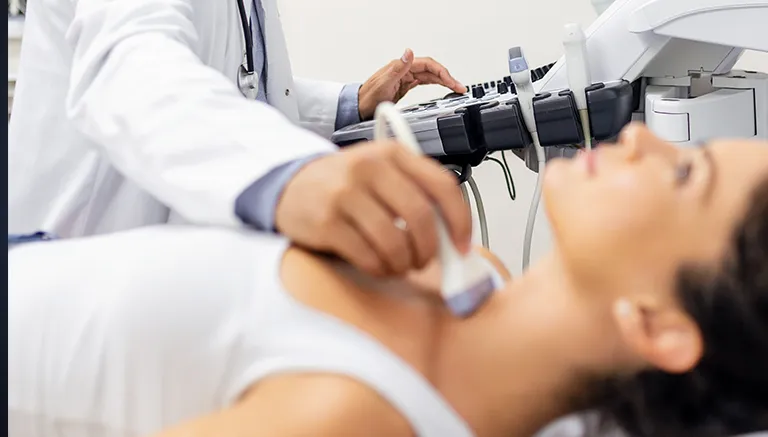
Echocardiography: Imaging the heart with the help of high frequency sound waves (Ultrasonography). Color Doppler Echocardiography, which is the functional test of this test, evaluates the pumping rate of the heart, the movement of the heart walls, clots within the heart, the condition of the valves between the heart cavities, the amount and type of fluid around the heart, the condition of the pericardial membrane surrounding the heart, and the structure and diameter of the vessels leaving the heart. makes.
Compiled by: Associate Professor Selvin Aydin